
Elodie 12-24 months: starvation mode, infantile anorexia, PPD & PTSD
After Elodie’s first year (where we started encountering feeding issues), at her first birthday she wouldn’t drink from the bottle anymore. Until then, we were still dream feeding her. Gradually it took 1.5 hour for her to just drink 40cc and then it diminished to just 20cc. The past six months we had been working really hard to teach her how to drink from a cup. Unfortunately, she couldn’t drink sufficient amounts from a cup yet. In order for her to drink enough we would spoon-feed her around 600cc a day because she was barely eating anything else.
Elodie kept sleeping in our arms, the minute we tried to lay her down she would wake up. As this was not our main problem we decided to let it be. It was actually the only moment when I could look at her without having anxiety or other negative thoughts.
Spoon-feeding milk
The spoon-feeding wasn’t quite easy to do. She would be seated, with the television on and was actually force fed until she had the minimal she needed to have. Her head would turn away and it took some serious ninja moves and sore arms to feed her.
There were many discussions about how to feed her. What was the best way?
It caused frictions. Other people couldn’t understand our situation. How our life looked like. It was all about feeding her. The minute she was awake we had to start feeding her. As no doctor listened and acted upon our worries, we didn’t have any other choice.
Silence please
She didn’t have much downtime to do other things, neither did we. We had to eat when she was asleep. I dropped food on her occasionally. While she was asleep it had to be really quiet, otherwise she would wake up. We sat on the couch with her in our arms, luckily our living room is spacious seeing the hours we had to spend here. Once I had to hold my pee for six hours because she was asleep and ill. We didn’t have the energy to change these things. Her sleeping time was a time for us to recover.
Bending over backwards to make her eat
Eating became more and more difficult, the speech therapist couldn’t really help us. We just had to keep offering her food, but the tiniest piece would make her vomit. We had to distract her extremely in order to be able to feed her, giving her all sorts of toys, so she wouldn’t push our hands away or refuse food in another way. She was still getting the fully puréed foods because she couldn’t handle the slightest chunk. The next months would be all about, how to distract Elodie, so she can eat.
It was difficult, how do you feed a child who already starts crying and fighting you when she had to sit in the high chair. There was absolutely no interest in eating. Something so basic.
I would think of the weirdest things, to get her to eat. I was in the supermarket with her 3 times a day, so she would eat. She would sit in the cart and I could feed her. Eventually we drove to other shopping centres to feed her. Something new, other distractions. Other objects I could put in her hands to distract her. I didn’t care what other people were thinking any more, I had no choice.
Good weather please
When the weather got better we would feed her in her high chair on the street in front of our house. People looked at us, judged us, but I had no choice. Some actually took the time to talk to me, and listen to my story. We became a phenomenon in our neighbourhood.

At least if we went out the house to feed her, it didn’t take us an hour to clean it afterwards. Our kitchen looked like a war zone after each meal. The entire day was about feeding, cleaning, and sleeping. There was no time left for other things. The thought of feeding her gave me panic attacks. Random things would cause me distress, like the thought of going outside the house, to talk to people. I couldn’t speak a sentence without ugly crying. Seeing that it would be raining the next day gave me panic attacks. How were we supposed to feed her now?
No health institution took us seriously. They said, ‘her weight is fine, don’t worry.’ What else could I do to keep my child alive? We had to keep thinking of ways to make her eat. Our one-year old didn’t understand that eating was crucial to stay alive.
Post-partum depression
During routine check ups we were still told that we were doing well, her weight was okay, and we should keep doing what we were doing. Our worries and stress weren’t heard or seen.
GP
I visited my GP in December 2019, and told her how I felt, what our home situation looked like, crying uncontrollably. She brushed it off as: ‘it’s just a bit of stress, it’s normal amongst new mums. It will be okay, give it time’.
A few months later when it became really apparent that I was in a very bad mental state, she apologized for not asking more and not seeing the signs.
The first person who really listened to my story was our corporate doctor, beginning of February. He told me that it seemed like I have a post-partum depression, and asked me to check up with our GP.
Mental health in Chinese culture
I was a bit dumbfounded when I heard his diagnosis. How could I have a depression, I have been through so much in my life, I am a strong, independent career woman. Mental health is not discussed in Chinese culture.
Talking about mental health and getting treatment is mostly hindered by strict social norms, and its subsequent stigma’s in Chinese culture. Add up to that the religious and cultural beliefs and regarding personal reputation and social harmony.
So needless to say I didn’t get much support from my own parents as they didn’t understand mental health. This was very painful and it really saddened me. Luckily my Belgian parents in law, were very kind, patient and understanding. They really helped us a lot. Just being there, helping us out without giving unsolicited advice.

GP’s assistant listened
After talks with the nurse practitioner and a medical visit with the GP’s assistant because Elodie was sick again, I was fast tracked to the psychiatric department in the hospital. The GP’s assistant was in shock when I told her my feelings, that I really had issues controlling myself, I was feeling really emotionless, so numb, and even had other scary, dark and very morbid thoughts. She called me a few days later to check up on me, and told me she was quite frightened and worried about me after my visit.
That visit snowballed my treatment. I received outpatient treatment for my diagnosed post-partum depression because it was important for my mental health, and for my family to not be separated from Elodie. The psychiatrist proposed anti-depressants but pointed out that I could go through an even worse (adjustment) phase before it gets better. The main stimulus of my depression, Elodie’s eating disorder could not be taken out of the equation, so anti-depressants would be like a bad band aid. I decided that I would not take any medicines, my family couldn’t take more than this. Even the thought of it gave me panic attacks. At least, without anti-depressants I understood where my emotions came from. I didn’t feel I could trust or understand my feelings on anti-depressants, besides that I have an addictive personality. I didn’t want to take any risk.
I know now that Elodie’s eating disorder, or infantile anorexia is not the only cause of my depression. Many other factors like my Chinese upbringing, and other life events contributed to that too. My, ‘get over it, it’s not that bad’, attitude didn’t give me time to heal over painful experiences. Then it builds up until everything crashes down.
Outpatient treatment
The psychiatric treatment has been an interesting journey as well. At first, a medical nurse came to our house every week to check on us. We really clashed, she was quite judgemental about us, about Elodie, her eating disorder and other behaviour. She felt useless because we had a really tight daily structure already. I was not the typical psychiatric (sometimes helpless) patient. I didn’t fit her idea of a helpless patient whom she could save. Her way of working and personality really triggered me, she was really dominant and only her ideas were correct, so we weren’t a good match. She did see that our situation was incredibly bad, and she told the psychiatrist that either Elodie or me was going to end up in the hospital. Unfortunately, she was not able to pull any other strings and get Elodie the help she needed. At one point she even mentioned that she had contemplated to bring in ‘Veilig thuis’ (child protection services) because she was worried about us. This shows how medics misunderstand the situation, we need help with Elodie’s eating, we need the right therapy. But instead they come up with stuff that we don’t need and would make matters even worse.
The difficult part about the mental health help we were receiving was that a child with an eating disorder, infantile anorexia to be specific, is not covered in their area of expertise. This was the crucial part that was taking us down. It was ruining our lives. I was psychically, emotionally and mentally exhausted. The eating problems were so overwhelming, you are so powerless and nobody understood or listened. The impact on us mentally was very much underestimated. I was a ticking time bomb.
Elodie received her own psychiatrist as well. They came by for an hour every week and leave. Still, after weekly visits they still didn’t see how much we were suffering.
Friends, and medics talk about self care, and how it will make you feel better. But I couldn’t think about self care, there was no energy for it, and I couldn’t enjoy it with an the worries I had. If I would be alone I would go nuts with my thoughts and sink further. I barely got through the day. I looked like a dirty cloth because after every meal I would be full of food stains, and I definitely didn’t have the energy to change clothes 4 times a day. I would see other toddlers all dressed up, matching clothes and cute. Their mums looking radiant and happy, with nice hair and make up. While I was already happy that I survived another hour, and managed to change her clothes 4 times a day, because she would be dirty and wet after each meal. We didn’t even use bibs, but used folded dish cloths because there would be a bigger chance she would remain clean. I didn’t want to go to sleep because after sleep comes a new day and I didn’t know how I could get through it…
And another depression in the family
My mother wasn’t at our house anymore by May because the feeding problems and tensions in our house, amongst other reasons, resulted in her becoming severely depressed. She and I in the same house, under these circumstances and with me being on sick leave was very detrimental to our relationship and my mental health. My mother was going to be admitted to a clinic where she would get treatment for six months. She is still recovering. We can earnestly say that the Elodie’s eating disorder was super detrimental to our well beings.
The sad part about this is that when I was diagnosed with my post-partum depression she didn’t take it seriously. She didn’t change her erratic behaviour and didn’t take my mental health into account. Our relationship is still difficult due to all the above. As I mentioned before, mental health problems are not acknowledged in Chinese culture. This had a very negative impact on my depression.
Raised temperature
Since her vaccinations in April, Elodie had been sick a few times and her temperature was always around 38.5 degrees. We went to the paediatrician in the Máxima Medische centrum in Veldhoven. They did some check ups and didn’t see something wrong. Her eating was getting worse. When we told the paediatrician our concerns he brushed us off. I was totally upset about the situation and crying my heart out. He said, ‘Her weight is within range, keep doing what you are doing. It’s fine, don’t worry, you are doing a good job.’ Saying that we couldn’t take it anymore didn’t matter. Basically, if she was almost dying we would be welcome to come again. We were in contact to see the eating team from this hospital, but there was no date confirmed yet. He told us to wait and see.
At the beginning of June we were at an all-time low. There was a whole circus act we had to perform to make Elodie eat. My father-in-law helped us out a lot and saw our struggle, our breakdowns, and he told my mother-in-law that we were not in a good place and something bad was going to happen if we didn’t get the help we needed

Well, something bad did happen. Elodie stopped eating and drinking fully. After 2 days I was going crazy, I called all the child care agencies that were involved, and they came to our house. I couldn’t do anything else but act and cry hysterically. I couldn’t take it anymore we needed help now, otherwise we would go insane! This was the point ever they finally listened. They later apologized for not seeing the signs and for downplaying our problems.
Emergency admission
Elodie was immediately admitted into the hospital, Máxima Medisch Centrum in Veldhoven where she had been before. She would stay here for almost a month.
The first night nurses wanted us to sleep apart, so I could rest. I told them, ‘No, I like to co-sleep, it calms me down. Also, Elodie still wakes up a few times every night. I can sooth her, so she falls back asleep quicker.’ They really pushed me to try the independent sleeping, so I caved, I was mentally unstable and a wreck. Of course, I didn’t manage to sleep at all. At around 03.00 in the morning I heard Elodie crying. After a while they went in to sooth her, and after an hour they came to get me because she wouldn’t calm down. I had told them about it, I know my child. On which planet is it a good idea to let a baby sleep in her own in a new surrounding, in a hospital?! Especially forcing it upon the parent. After this night they let me sleep with her. We slept together on the couch, it was really cramped. I put a chair at the end of the bed, so I had a bit more space for my legs. Luckily Elodie was still small enough so this could fit.
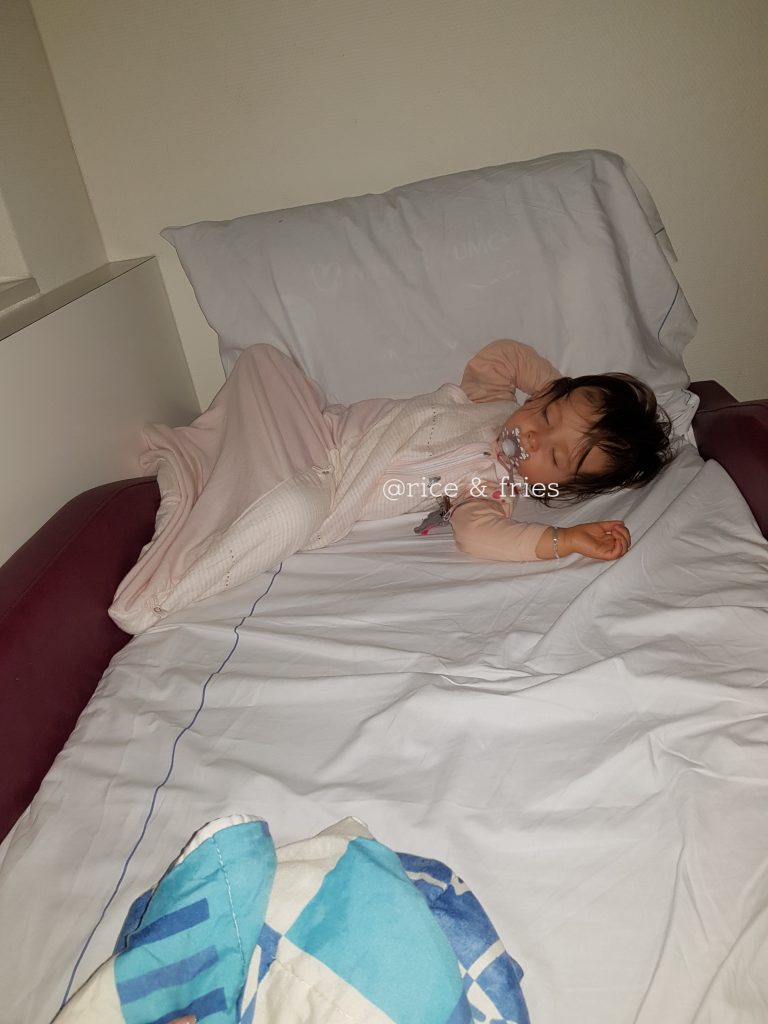
9 day hunger strike
The hospital admission did more bad than good. Their goal was to ‘break’ Elodie, so she would start eating and drinking, an extreme hunger provocation (which might work for ‘stubborn’ children or picky eaters). Instead of a hunger provocation it was truly more starving her and hoping she would eat. Elodie didn’t eat and hardly drank for nine days. She drank the bare minimum to prevent dehydration. The entire month in the hospital she barely had wet nappies and her poop came one of two times a week. Whereas normally she would poop multiple times a day.
Tube in sight
If she wouldn’t start eating after the ninth day of not eating she would get a tube. The 10th day she ate a tiny bit. The tube was postponed because doctor wanted to prevent it if possible, which I understood.
When she started eating it wasn’t even a spoon full of food the entire day. Yet, they were cheering how great she was doing. We became quite allergic to this behaviour, the fake optimism and cheerfulness to distract us from our problems.
At some point Elodie got a rash and I suspected a food allergy. Yet, they could see it was nothing, they could also see she was perfectly fine and healthy, while eating nothing. An interesting way of diagnosing diseases. Even though we told them she is much more lethargic than at home, she was so unwell that she wanted to be carried. They would tell us that we spoil her too much, and she should walk on her own. We should tire her out so she would eat. It never popped their arrogant, know it all minds that she didn’t have the energy while living off only 5 peas a day and half a glass of milk.
Parent blaming
They wouldn’t hear us out. Her eating habits were our fault. If we wouldn’t worry so much she would miraculously start eating. Everything was our fault, and we did many things the wrong way. The paediatrician was trying to talk me into anti-depressants, telling me how great they are. Like it’s some sort of magic pill. Sorry, you are not my psychiatrists and you are telling me what I should take? So I asked her whether she had ever taken them herself. The answer was no. So I told her to stick to her own profession, and that I absolutely didn’t appreciate her trying to be my psychiatrist. Even the nurses were talking about how great anti-depressants were. I had to tell them that they were not in the position to discuss this with me. It’s not like anti-depressants would solve Elodie’s eating problems.
A month later she was discharged, they couldn’t help any further. Their arguments were contradicting each other on many points, when we highlighted this there came another excuse. The paediatrician was twitching during our talks because we were so on top of everything she was saying. That she was eating so little was fine, the paediatrician said, ‘Kids this age can live of the air, if she doesn’t gain any weight in four months contact us again.’
We were brushed of as ‘those parents’, the annoying, irrational, and hysterical ones. We were sent home while Elodie was having a stomach flu, eating almost nothing, she went from 10.3 kg to 9 kg. She would drop to 8 kg less than a month later.
They assigned us family coaches to change our behaviour, because from their perspective it was all our fault. The family coaches and our other child care agencies were told that it was us, causing Elodie’s eating problems. If we were fixed, Elodie would magically start eating like a normal child. This really caused some rifts between us and the child care agencies. It was us against the world, the institutions that should help us were brainwashed by the know it all and vain paediatricians. The family coaches quickly found out that we were not at the core of the problems, but Elodie really didn’t show any interest in food. They had never seen anything like this before. She was getting sick very often and was losing weight so quickly that they got worried as well. By August, she was barely weighing 8 kg, at 19 months old.
We got a second opinion at the hospital in Turnhout, Belgium, they did a blood test which showed she had an egg allergy. After that incident, and Elodie’s continued eating problems the hospital in the Netherlands, MMC, obliged to run some medical tests, additional blood tests, a scan to check her swallowing and reflux, and an internal echo. Nothing came out of these tests. We were glad nothing came out but still we didn’t have a diagnosis.
Medical nutrition
In order for her to at least get calories we pushed the dietician to give Elodie medical high caloric food. The hospital apparently prohibited it, because according to them Elodie was fine, we were just crazy parents. After our second visit she subscribed the medical nutrition. We had noticed that the hospital’s paediatricians vision was clouding opinions of other specialists and child care agencies. They were afraid to follow their own instincts. So, even though Elodie was released from the hospital, weeks later we were still feeling their influences.
Elodie’s body in starvation mode
The dietician explained that the extreme hunger provocation, which actually was more like starvation, in the hospital led to Elodie’s body going into starvation mode. She barely needed calories to survive, she didn’t feel hunger, and she didn’t want to eat. So the situation was actually worse than before. Luckily she was still growing, so the food that she ingested was used to its maximum.
We were at wits end. In order to make her eat at least something, I took her out on walks and while she was waking I was feeding her. Then that wasn’t distracting enough anymore, and she would walk around in the supermarket while taking products from the shelves while I was feeding her. Some people bought some products with Elodie’s food stains on it for sure.
I fed her while she was playing in the bathtub. She couldn’t get away, and she was playing and distracted. The water was incredibly dirty afterwards, so I still had to wash her before she could come out of the bath. According to the family coaches I was very inventive in thinking of ways to get Elodie to eat. Again, we had no choice, and we wanted to prevent a tube.
By October, I would have to go outside to feed her while walking three times a day. I even went to different supermarkets in one day so the staff wouldn’t recognize us. It was extremely straining and very stressful.
We were spending a lot of money every month on extra groceries hoping there was something she liked to eat (we still do). There was nothing that would spark her interest.
NoTube
Online we found information about NoTube. A non-profit organization with a group of paediatricians whom are highly skilled in tube weaning and helping children with eating problems. Unfortunately it wasn’t covered by our health insurance. My husband’s new car had to wait a bit longer. This was our last resort.
No other options
The options in the Netherlands didn’t fit our family. They either see your child for half an hour a day, or you are separated from your child for a longer period of time, or the waiting list was years. This was not an option for us. Elodie was too young for those options, it would influence the already difficult aspect of bonding, and we couldn’t wait years to get help.
Our NoTube adventure is discussed in other posts. We were so happy we went. This was a lifesaver, although the time there was still quite stressful, especially in the beginning. Elodie was really happy there and started ‘sipping & snacking’. We were taught about how Elodie feels about food, about her infantile anorexia, and how to help her be more comfortable around food. It boosted her development. Feel free to contact me if you have any questions about the therapy at NoTube.

Finally, no more parent blaming
Most of all, we were heard, we were treated as human beings and treated equally and with respect. That was at least one aspect that was not causing us additional stress. The team is super knowledgeable, arguments are evidence based and their approach is custom, it fits the specific child. They would not let Elodie lose too much weight, and they would monitor it. We were treated as a family because it is a problem which affects every family member. The paediatrician Dr. Scheer was with us every meal, and we had many information and learning to eat sessions. In the end we actually enjoyed our stay there, Elodie was making a little progress, and she loved playing with the other kids. She had never played with other children before, it was simply not possible, we didn’t have the energy or possibility because of her eating disorder. We didn’t even have spare time for ourselves.
We were told that parent blaming was a very regular practice by medical professionals. Especially if there are no other medical issues, then it was certainly the parents fault. They saw it happening to other families coming to NoTube all the time. This parent blaming left me incredibly insecure about parenting, we were traumatized and my anxiety was at an all-time high.
Infantile anorexia
It was also a relief to have a diagnosis, extreme food aversion a sort of infantile anorexia. It was nice to be able to give Elodie’s eating disorder a name. The minute other people started saying their children were picky eaters too, we just mentioned infantile anorexia. That was enough. We didn’t need to defend ourselves anymore, we were not brushed off or not taken seriously anymore. It was such a relief. We were not crazy, irrational and whatever else professionals and maybe even friends were thinking of us. I was hysterical though, but I believe that’s justified as nobody would listen to us.
Baby steps
After attending the NoTube eating school, Elodie was starting to make a little progress. We learned to understand her world, a world in which she knew how and what to eat. It was not enough to survive or thrive on her own, but she was showing interest in food sometimes. It was still ‘sipping and snacking’ but that was already a vast improvement. We were getting out of the extreme food aversion state.
After the NoTube EAT Campus we received three months of telemedical aftercare, where we had daily contact. They also actively followed up on Elodie development.
In December Elodie started to go to play groups at a daycare, once a week for 1.5 hour. Due to her very low body weight (at the bottom of extremely underweight) and her diminished immune system she was starting to get sick all the time. This had a bad impact on her autonomous eating, she was losing weight and was barely 9.5 kg at two years old, and was still wearing size 80, for more than a year already. We stopped going to the play groups as this was ruining everything we were working on. Now, we could fully focus on helping Elodie. If Elodie would get better, we would get better too.
Malnourished
She was all skin and bones, no cute baby fat on her body and she was failing to thrive. Needless to say that during this period we mentally pretty much hit rock bottom as a family. Seeing her sparse and brittle hair, nails not growing, bony ribcage, and being able to count her vertebrae, was a daily reminder of the fact that Elodie was severely underweight and malnourished.
It was terrible, I wanted to cry every time I saw her. I wasn’t the only one, when my husband saw pictures from a year ago when she still looked chubby he was having a very hard time as well. Which parent wouldn’t? Whenever I saw other children who looked healthy, I got sad and jealous. How long would it take for little Elodie to pass the sipping and snacking phase?
Other people couldn’t see that we had a special needs child. They saw a normal child who is happy because she was wearing a body warmer during the colder days because she got so cold, yet she had chubby cheeks. So she looked okayish. When a family coach picked her up she was shocked at how skinny Elodie was, she told me it didn’t look that bad until she felt all her protruding bones. It was a horrible period in my life as a mom, I was so absorbed in my worries that I couldn’t enjoy being a mother.
Ronald McDonald’s home
While Elodie was hospitalized there was a lady working at the Ronald McDonald’s home who also had a toddler with terrible eating problems many years ago. She told me that her daughter later got terminally ill, and people were supportive and kind to her at that time. Whereas the period where her daughter was not eating was just as bad for her mental health, but people didn’t treat it like something important, they were not supportive even though it’s also life threatening. She told me that period was even worse, because she needed acknowledgement and support. The quote, ‘Don’t judge a book by its cover’ really applies to invisible disorders.
We had a great time at the Ronald McDonald’s home. What a great organization with wonderful and lovely people working there. We are really grateful for their existence, it made our time at the hospital bearable. We met other parents who each faced their own issues. Although the problems were not the same it was nice to talk to other parents because somehow you are still alike. Most of the volunteers have their own story to tell as well. Because we were there for such a long time we got to chat with them and learn their stories. It was very enlightening.




